|
September 2014, Volume 36, No. 3
|
Dr Sun Yat Sen Oration
|
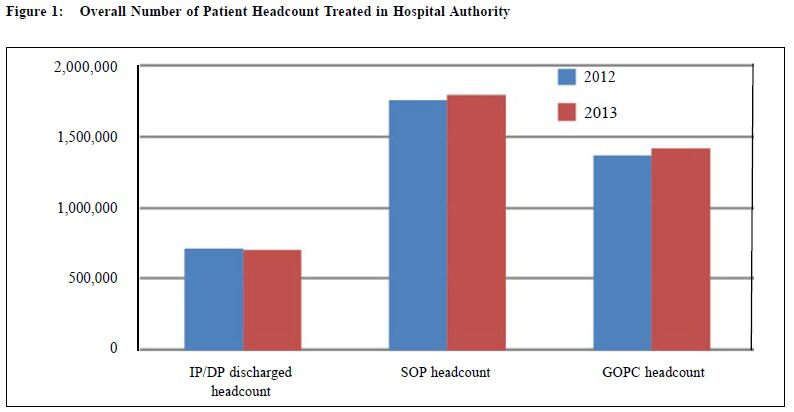
Delivering medical care – attempt to think out of the boxJohn CY Leong 梁智仁 HK Pract 2014;36:99-102 It is generally acknowledged that Sun Yat Sen is the father of modern China. What is not that often acknowledged is that he played an important role in the introduction of Western Medicine into Hong Kong, and in turn, to China. This was, in part, achieved by his being educated in the art and science of Western Medicine when he was one of the two first graduates of the Hong Kong College of Medicine in 1887. Twentyfive years later, the University of Hong Kong was established, with the Faculty of Medicine as one of the three founding faculties. Dr Sun was a general practitioner in the widest sense, because there was certainly no specialisation in those early days. A hundred and ten years later, the Hong Kong Academy of Medicine was established, opening up the formal training and accreditation of medical specialties. General practice has taken on a new meaning, and it has become recognised that a period of formal and well-planned supervised training, after undergraduate education, is needed to enhance general practice of medicine to the specialty of Family Physicians. The reason why the colonial British Government in the 1880s decided to set up the Hong Kong College of Medicine was that the Chinese population at that time almost entirely consulted Chinese Medicine practitioners for their illnesses. Only when their illnesses were so serious that Chinese Medicine was unable to deal with that they sought help from Western Medicine practitioners. The latter were almost entirely Caucasians, rendering communication between doctor and patient difficult because of the language barrier. The then Government took a wise decision to start an institution for education of the Chinese population in the art and science of Western Medicine. This was the beginning of a public medical service for in-patients as well as out-patients. Fast forward to the Post Second World War era, the public medical and health service was under the authority of the then Medical and Health Department. The main mission at that time was the need to safeguard and promote the general public health of the community as a whole; and the need to ensure the provision of medical and personal health facilities for the people of Hong Kong, including and particularly that large section of the community which relied on subsidised medical attention. The gradual but sustained immigration into Hong Kong from the Mainland after the establishment of the communist regime continued to put heavy pressure on the public medical service. Although the medical care was of international standard, the facilities and hardware of public hospitals were below par and could not catch up with the ever increasing volume of patients. The formation of the Hospital Authority in 1991 was a commitment by the then Government to upgrade all aspects of the public medical service. Indeed, it has achieved much towards that goal. However, in some ways it has become a victim of its success. The subsequent presentation and discussion of this oration will refer to only the in-patient aspect of the public medical service. It will highlight the existing pressure in terms of demand (Figure 1 & Figure 2) and projected requirements to the next decades, the hardware and facilities required to satisfy the demands of a growing population, and an increasing percentage of the elderly population (particularly the so-called "Old Old", i.e. people over the age of 80 or 85).
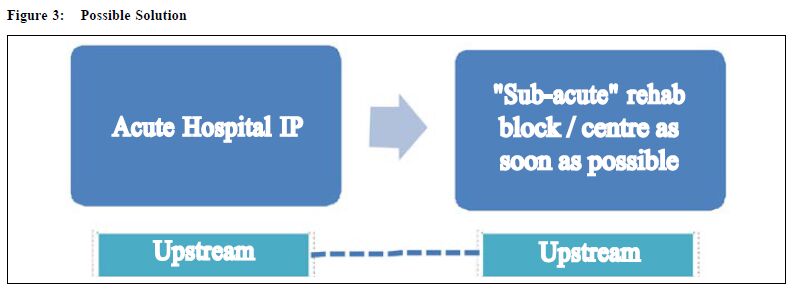
The oration will attempt to suggest looking at ways other than the present established modes of planning to deal with the ever increasing demand. Ideas to be discussed include the shifting of certain types of patients occupying acute hospital beds to subacute rehabilitation beds in rehabilitation blocks near to acute hospitals (Figure 3 & Figure 4), concomitantly upgrading of the nursing care in the rehab blocks to be able to handle these subacute patients.
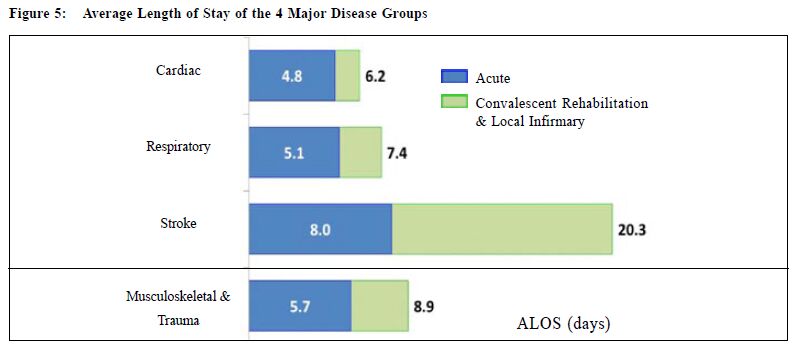
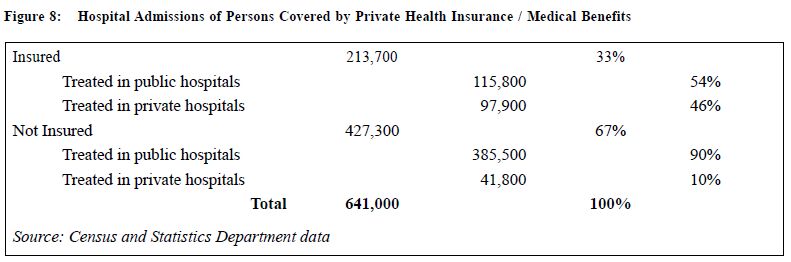
Examples will be given of the average length of stay (ALOS) of the most commonly admitted groups of patients in the Medical & Geriatrics Ward, i.e. respiratory, cardiac, and stroke (Figure 5). Estimations of how reducing one-third (Figure 6) and half (Figure 7) of the ALOS can theoretically vacate a significant number of beds in acute wards for emergency admissions. Discussion will be offered as to how patients, with privately purchased medical insurance or medical service provided by employers, presently being treated in the public acute hospitals (Figure 8) can be shifted to private hospitals (Figure 9). Also, how to attract Family Physician Fellows not only to work within the public medical service, but to mentor general practitioners to become competent enough to deal with the large volume of patients with chronic diseases to shift them from Specialists outpatient clinics to the General outpatient clinics. It is argued that thinking out of the box, rather than just following established planning policies and procedures, can contribute towards coping with the high demands of the public medical service.
John CY Leong, DSc, MBBS, FRCS, FHKAM
Chairman, Hospital Authority Correspondence to : Prof John CY Leong, Hospital Authority Building, 147B Argyle Street, Kowloon, Hong Kong SAR, China. |
|