Research & Publications > The Hong Kong Practitioner > Clinical Quiz

Clinical Quiz (Please login 'Member Area' for online submission of latest issue)
Clinical Quiz June 2024
A 6-year-old boy with good past health complained of itchiness over his scalp for 3 months
Dr. Adrian KC Cheng
|
Readers are invited to participate in the Clinical Quiz*. Simply answer the question, fill in the reply slip and return it to the College by 22 Aug 2024. Each reader is allowed to submit one entry only.
*Note: There would be no prize award for this issue while sponsorship for Clinical Quiz has been ended in September 2020 issue. The answer of the Clinical Quiz for this issue will be announced in the next issue. Thank you for your support.
|
Clinical history:
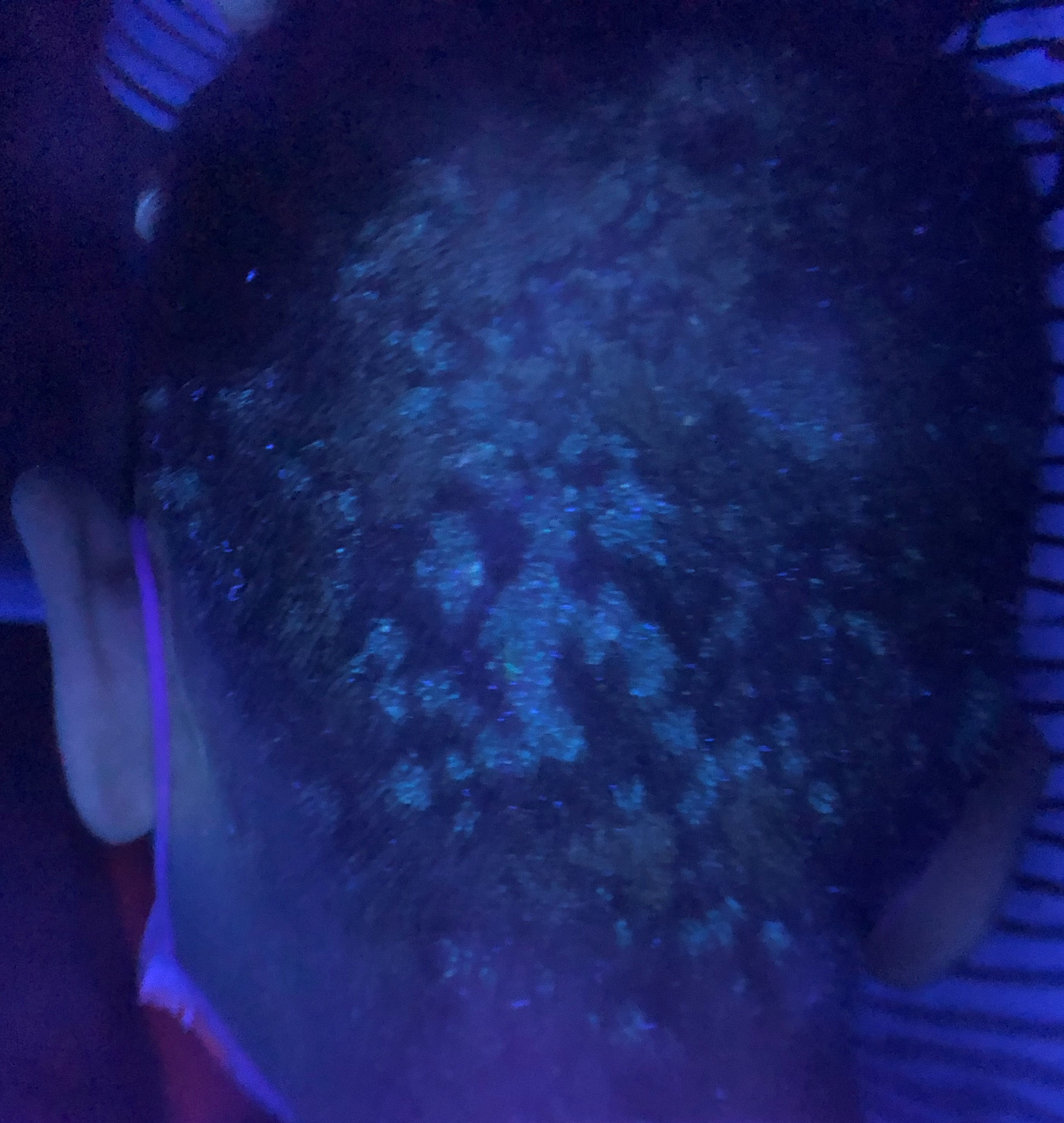
A 6-year-old boy with good past health complained of itchiness over his scalp for 3 months. Clinical examination showed erythematous scaly plaques over his occipital scalp and posterior neck with occasional pustules. Wood’s lamp examination (Ultraviolet lamp) showed green-florescence over the lesions. There were no other lesion over his face, trunk and limbs. Nails examination was normal.
What is the diagnosis?
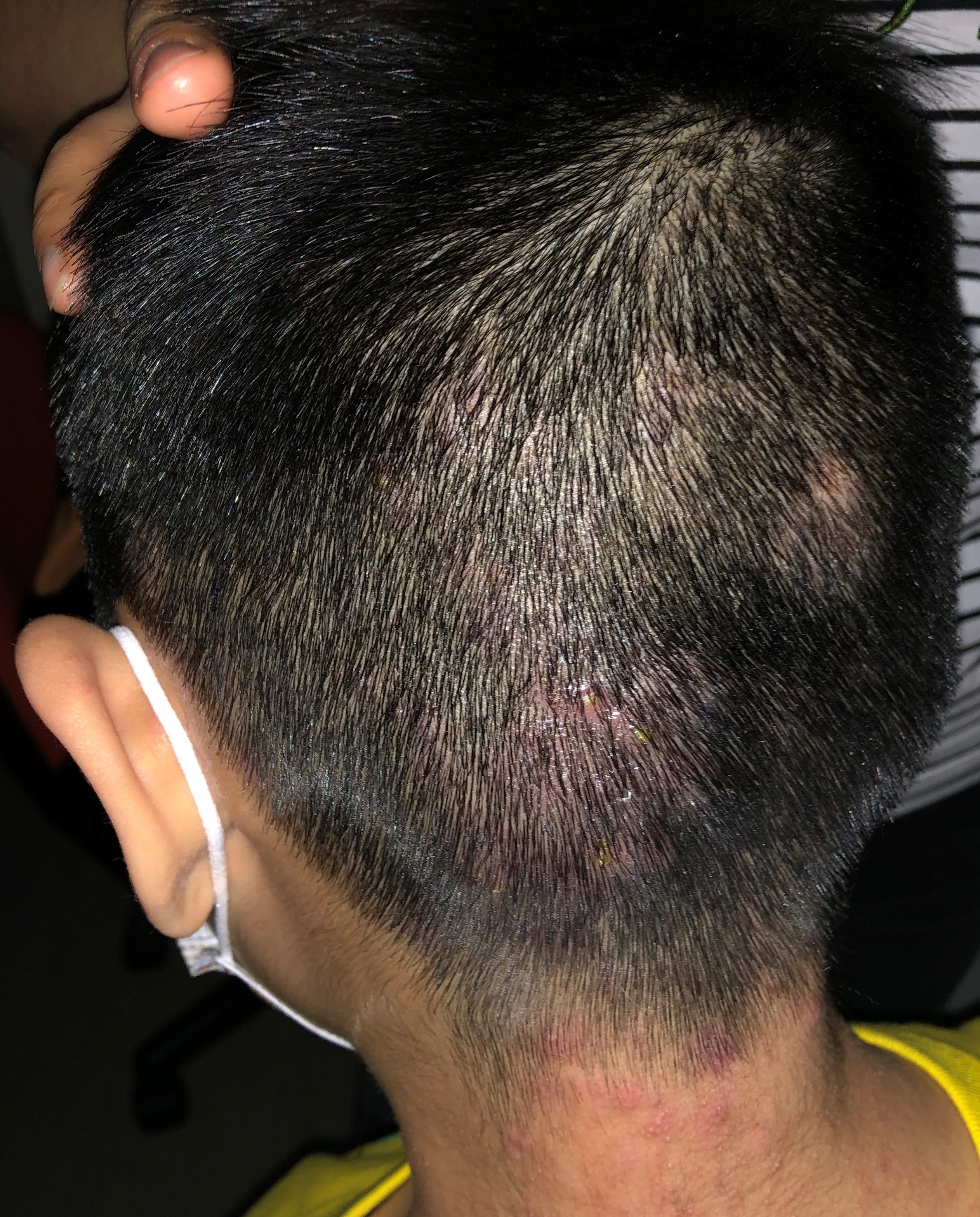
| A. | Seborrhoeic dermatitis |
| B. | Tinea capitis |
| C. | Pustular psoriasis |
| D. | Lichen planopilaris |
| E. | Alopecia areata |
Answer:
B. Tinea capitis
Tinea capitis, or scalp ringworm, is dermatophytosis of the scalp. Unlike other dermatophytosis which is most commonly found in postpubertal individuals, tinea capitis occurs primarily in children. Tinea capitis can be inflammatory or non-inflammatory. Non-inflammatory scaling resembles seborrheic dermatitis. The range of clinical presentation ranges from mild scalp scaling, to patchy alopecia with scaling and black dots, to large alopecia patches with pustules. Inflammatory tinea capitis can result in a severe pustular reaction with alopecia and boggy purulent plaques known as kerion, due to exaggerated immune reaction to dermatophytes. Patients with tinea capitis may also have posterior cervical and posterior auricular lymphadenopathy.
Wood’s lamp examination displays yellow-green fluorescence in ectothrix invasion pattern by certain Microsporum species, such as Microsporum canis. Dermoscopy may reveal typical findings of “commalike” or “corkscrew-like” broken hairs that represent clues to the diagnosis of tinea capitis.
Microscopic examination of plucked hairs in the involved areas after application of potassium hydroxide may reveal fungal spores within or outside the hair shaft for endothrix and ectothrix infections respectively. Plucked hairs can be sent for fungal culture but culture results may not be available for several weeks. Treatment is usually started empirically based upon the clinical diagnosis to prevent complications such as alopecia.
Griseofulvin appears more effective than terbinafine for Microsporum infections. The recommended treatment duration is 6 to 12 weeks. Griseofulvin is the first-line treatment for tinea capitis in children in whom the culprit organism is unclear. Both griseofulvin and terbinafine are accepted first-line treatments for known or suspected Trichophyton tinea capitis.
The slide and the question were prepared by:
Dr. Adrian KC Cheng, MBBS(HK), MRCP(UK), MSc GEOR (CUHK), FHKCP, FHKAM (Medicine)
Specialist in Dermatology & Venereology;
Associate Consultant,
Division of Dermatology, Department of Medicine, Queen Mary Hospital, Hong Kong SAR
Back

